Thousands of dollars are spent each year by clinics due to the mistakes made when billing, especially when it comes to time-based therapy services, which are billed incorrectly. One of the most common billing guidelines to master is the 8 Minute Rule. 8 Minute Rule is a Medicare-defined standard that indicates how many units you are eligible to bill for timed therapy services. It is crucial to learn how to apply the 8 Minute Rule to minimize the risks of audits, denial, and loss of revenue when you are getting to know what medical billing is, training new therapists, or refining the revenue cycle management of your clinic.
This is an informative guide that helps you understand what the 8 Min Rule is, how it is differentiated from other payers, and how to prevent the clinic from experiencing the medical billing mistakes that risk your clinic.
What Is the 8 Minute Rule?
8 Minute Rule/8 min rule, and Medicare 8 Minute Rule are the same and refers to the same matter, which is the policy employed by Medicare and many other commercial payers in determining the number of billable units that can be submitted for time-based CPT codes in outpatient therapy.
This guidance mainly covers:
- Physical therapy (PT)
- Occupational therapy (OT)
- Speech-language pathology (SLP)
The intention is to make sure claims represent actual direct, one-on-one skilled care, as opposed to time spent on documentation, time spent on changing or preparing the client, time spent on breaks, time spent using passive modalities without the therapist being present, and any time spent not actively engaged.
Comprehension of the 8 Minute Rule is necessary in order to obtain the best and cleanest bill possible, have the least number of claims be denied, and receive the most effective and accurate services possible from the revenue cycle management services.
Why the 8 Minute Rule Matters for Your Practice
Billing correctly under the Medicare 8 Minute Rule affects:
- Reimbursement accuracy
- Audit protection
- Financial well-being of the revenue cycle
- Denial prevention
This allows your practice to operate like the best medical billing companies or to provide a better experience when outsourcing to professional billers, helping with clean claims and with better denial management.
How the 8 Minute Rule Works
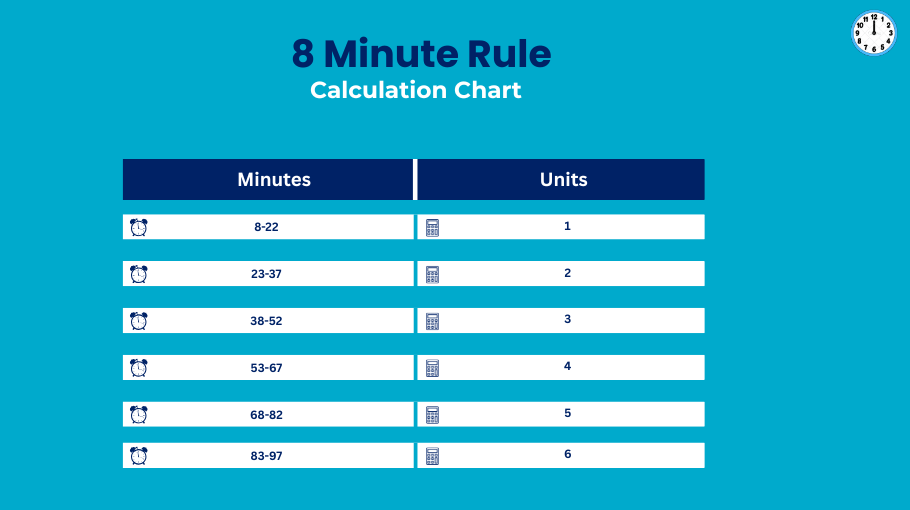
The 8 Minute Rule is based on 15-minute increments, meaning that each block of a billable unit is 15 minutes of direct treatment. This means that therapy should usually be calculated in blocks of 15 minutes. However, in order to make the practice easier, a threshold was introduced that allows a unit to be billed provide that at least 8 minutes of skilled care was used.Per Medicare guidelines:
- 8-22 minutes = 1 unit
- 23-37 minutes = 2 units
- 38-52 minutes = 3 units
- 53-67 minutes = 4 units
And so forth… Medicare billing guidelines specify that any service rendered that is less than eight minutes is not billable. This is why clinics document revenue loss: a therapist will document 5-6 minutes of a modality and fail to merge it with other therapeutic time. Understanding how to calculate total time and applying the 8 minute rule is crucial in avoiding the most common medical billing oversight.
Why the 8 Minute Rule Matters for Growing Clinics and Practices
Medicare compliance is necessary, however, the impact that the 8 minute rule has on business is undeniable. It enhances the efficiency of cash flow, helps in maintaining a healthier accounts receivables and overall enhances how the business operates.
The 8-min rule is the basis on which a predictably profitable revenue cycle is built. Those providers that properly incorporate Medicare rules into their documentation and billing practices experience significantly increased clean-claim rates. This, in turn, reduces the degree of payer documentation requests and increases practice efficiencies related to payer documentation, allowing clinician documentation to be focused on patient care. These functions define revenue cycle management and are the reasons why most practices that achieve operational efficiencies in revenue cycle management partner with leading medical billing companies.
Billing errors can lead to thousands of dollars’ worth of lost or delayed revenue on a time basis billing. Inaccurate billing for even one day has the potential to result in an audit. Also, one error in applying the 8 minute rule can lead to a gradual erosion of trust by payers. All of these consequences can be avoided, to a large extent, through the meticulous attention to detail the team has given to employee training and the outsourcing of denial management services.
Step-by-Step: How to Apply the 8 Minute Rule Correctly
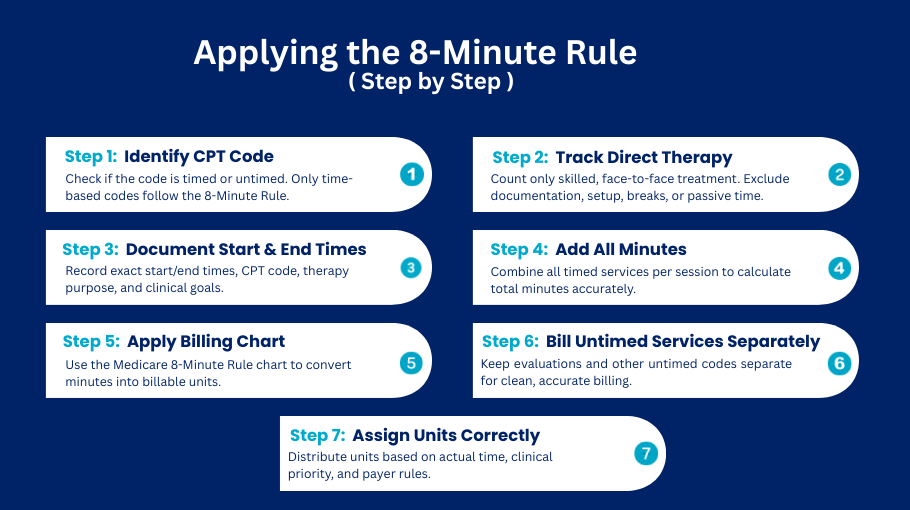
Step 1 – Determine if the CPT Code Is Timed or Untimed
Not every CPT code has an 8 minute rule requirement for billing. Time-based codes must adhere to the rule. Untimed codes do not have to follow the 8 minute rule.
Examples of time-based codes:
- Therapeutic exercise (97110)
- Manual therapy (97140)
- Neuromuscular re-education (97112)
There are untimed service-based codes, which are evaluative and some modalities, which are not subject to the 8 min rule.
Step 2 – Monitor One-On-One Direct Treatment Time
Only skilled, one-on-one face-to-face treatment is applicable to the 8 minute rule.
Exclusions include:
- Documentation
- Equipment setup
- Rest breaks
- Passive modalities (unless there is direct involvement of the therapist)
- Waiting time
Step 3: Document Start and Finish Times for Every Service Provided
Ideally, documentation should be performed for audit preparedness and for reimbursement purposes.
Always note:
- precise start time
- precise end time
- applicable CPT code
- reason for service
- clinical result or objective
The top clinics, like any top medical billing company, are clear that proper documentation is the cornerstone of successful billing.
Step 4: Sum all billed time-based minutes
The 8 Minute Rule is often the most misunderstood of all medical billing tasks.
You must sum all time-based, one-on-one service minutes billed per day, per discipline.
Illustrative Example:
- 10 min manual therapy
- 12 min therapeutic exercise
- 9 min ultrasound
- Total = 31 min -> 2 billable units
Failing to sum times is one of the most prevalent mistakes made in medical billing.
Step 5: Use the 8 minute Rule Billing Table
The following is the unit calculation chart of Medicare:
- 8-22 minutes -> 1 unit
- 23-37 minutes -> 2 units
- 38-52 minutes -> 3 units
- 53-67 minutes -> 4 units
- and so forth
This is the essence of the Medicare 8 Minute Rule and is critical to avoid having claims denied.
Step 6: Bill All Untimed Services Separately
Time-based codes must always be billed in conjunction with untimed codes (evaluations, some modalities, etc.). Separating services results in cleaner billing and is beneficial in regards of keeping the revenue cycle smooth and in order.
Step 7: Assign Units to the Appropriate CPT Codes
After determining the total minutes worked and the units that can be billed to the client, assign units corresponding to the following:
- Total time worked
- Clinical work performed
- Payer rules
Proper unit allocation assists in avoiding incorrect billing, and enables the clinic to manage the denial of the billing in an efficient manner.
Common Mistakes That Cause Billing Errors

Mistakes happen, and with the 8-Minute Rule, even the most seasoned clinics run into problems. The following errors are the most common with the 8-Minute Rule.
Mistake 1: Rounding Time
If a service was performed for only 10 minutes, billing for 15 minutes is a common rule violation. It is a denial risk.
⭐ Avoidance tip: Time to the second, and use a timer to stay on track. Record actual clock-in and clock-out times.
Mistake 2: Counting Non-Direct Care Time
Including time when the therapist wasn’t actively providing care — like writing notes, prepping equipment, or waiting for a machine — is not allowed.
⭐ Avoidance tip: Keep track of when you stopped and when you started with the other tasks.
Mistake 3: Forgetting to Add Multiple Time-based Services into One Service
When billing for multiple short time-based chunks of care (example, 6 min manual therapy + 6 min exercise + 6 min ultrasound), it may feel reasonable to bill “zero units” for each, but combining them may equal a unit.
⭐ How to avoid this: Always calculate the total billable time for each patient for each day (for each discipline) before rounding time entries to units.
Mistake 4. Incorrect distribution of units across billing codes
There are clinics that distribute units in a way that does not reflect to time spent or clinical value, as in, allocating all units to a code that is a lower value to secure more reimbursement.
⭐ How to avoid this: Allocate units to those codes that represent the highest value in terms of the volume or the most clinically relevant services. Check the payer guidelines that you are operating with to understand their policies on this.
Mistake 5. Confusing time-based codes with service-based codes
There are errors that come as a result of billing a service based (untimed) code as if it were time based instead, or the opposite.
⭐ How to avoid this: Keep a list of which CPT codes are time-based or not, and verify before finalizing billing.
Mistake 6: Insufficient or Inaccurate Documentation
Notes that lack timestamps and descriptions of the relevant therapy, such as, “did therapy for 20 min,” are likely to be denied or audited.
⭐ Strategy to avoid this: Use sufficient and accurate documentation; record the start and end times, specify the procedure or type of therapy, and provide a justification for the need of the therapy.
Best Practices — How to Avoid Mistakes and Stay Audit-Ready

Based on common pitfalls and guidance of the payers, here are best-practice suggestions for handling 8-Minute Rule billing:
Utilize time-tracking mechanisms
- In clinical sessions, consider employing a stopwatch or timer.
- If you can, use an Electronic Health Record (EHR) or Electronic Medical Record (EMR) system that automatically logs the time when a service starts and ends.
Retain a coding reference sheet
- Keep a record that differentiates which CPT codes are time-based from which are service-based.
- Review and keep it current regularly, as payer policies can change.
Document completely
- For every service that is timed, record the start time and the end time of the entire service.
- Specify the therapy or procedure performed (for instance, “Therapeutic exercise: 09:00–09:18.”)
- Short descriptions justifying the service should be included as they can be quite important for audits.
Exclude Not-direct-Care Team
For passive modalities, documentation is not to be counted, as well as time for equipment preparation, breaks, waiting time, and time where the therapist is not present.
Keep current with guidelines from payers.
- Variances might be present for private insurance and non-Medicare coverage.
- Even with Medicare as primary insurance, secondary coverage might perform audits, which is why documentation should be thorough and correct.
Review and Internal Quality Assurance
- Ensure that review of billing claims to utilize and confirm compliance.
- Perform time audit exercises to compare the total time recorded with the units billed.
- Educate therapists and billing staff on the Eight-Minute Rule.
How the 8 Minute Rule Impacts Revenue Cycle Management
Improperly billing the rule results in the following:
- Claim denials
- Lost revenue
- Take backs
- Increased administrative work
- Risk of audits
This is the reason why numerous clinics collaborate with the top-rated medical billing companies or tailored RCM partners.
The 8-Minute Rule in 2025 and Beyond — What’s New
For the several decades that the 8-Minute Rule has been in effect, its implementation and enforcement have not been the same, but according to the latest updated guidance available to us:
- Medicare and other payers have shown more focus on exact time tracking and documentation. Statements such as, 20 minutes of therapy are insufficient.
- The frequency of audits has been increased. Complete billing via overbilling is a common reason for recoupment of claim denials and compliance investigations.
- The tendency for clinics to switch is due to the use of integrated Electronic Health Records and billing systems that automatically log time spent on a service, compute billable units, and decrease any possibility of manual error
Consequently, 2025 and beyond is less about ‘getting away with sloppy billing’ and more about having documentation discipline, clarity, and preparedness for audits.
How Outsourcing Helps With the 8 Minute Rule

Error prevention is an area where professional billing companies and RCM partners shine. They assess,
- Compliance with the Medicare 8-minute rule
- Correct unit calculation
- Documentation Standards
- Specific Guidelines per payer
- Trends in denials
The right partner delivers:
- Rapid payments
- reduced denials
- less administrative burden
- better financial outcomes
This explains why clinics frequently depend on sophisticated denial management services to reclaim revenue lost to improper time-based billing.
Summary & Final Thoughts
The 8-minute rule may come across as an uninteresting billing policy, but its proper execution can significantly influence outcomes. It guarantees just compensation for rightful services rendered, mitigates audit risks, and maintains the trust of both patients and payers.
The most important take-home message here is to be precise, consistent, and transparent.
- Document only the actual time of care delivered.
- Aggregate all therapy minutes per session.
- Utilize proper starting and ending timestamps.
- Understand which of the codes are time-based and which are service-based.
- Accurate unit calculations, including logic for the remainder, are necessary.
- Clarity of clinical necessity must be documented.
With such practices in place, common billing pitfalls can be eliminated, and revenue can be optimized while staying compliant, for you or for your clinic. Armored MBS is here to ensure your billing stays accurate, compliant, and efficient—especially when applying the 8-minute rule.
Stop losing revenue to simple billing mistakes.
Partner with Armored MBS for clean claims and confident compliance.

TESTING